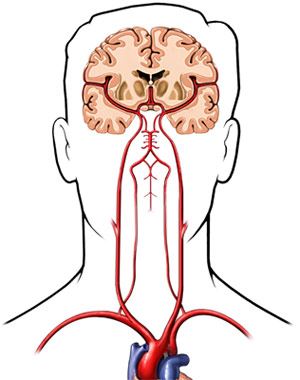
Syncope, also known as fainting or passing out, is a sudden and temporary loss of consciousness that occurs due to decreased blood flow to the brain. This can happen for a variety of reasons, including dehydration, low blood pressure, heart problems, neurological issues, and even emotional stress. The symptoms of syncope include lightheadedness, dizziness, blurred vision, sweating, and nausea.
While syncope itself is usually not harmful or life-threatening in most cases it’s important that anyone who experiences it seek medical attention to determine the underlying cause. Doctors may perform tests such as an electrocardiogram (ECG) or tilt table test to diagnose the condition and recommend appropriate treatment. Treatment options depend on the underlying cause but may include lifestyle changes such as staying hydrated and avoiding triggers that cause fainting episodes.
In summary, Syncope is a relatively common occurrence that many people experience over their lifetime- some more than others- but should never be ignored due to potential underlying conditions causing it. With early detection and proper management by healthcare professionals, this condition can be better managed for overall health benefits moving forward in one’s life.
Table of Contents
Types
There are three main types of syncope: Vasovagal, orthostatic, and cardiac. Vasovagal syncope occurs due to a sudden drop in blood pressure caused by certain triggers such as pain or emotional stress. Orthostatic syncope happens when there is a change in posture from sitting or lying down to standing up, which leads to decreased blood flow to the brain. Cardiac syncope results from an irregular heartbeat or other heart-related issues.
Reflex syncope is typically benign and may not require any treatment unless it occurs frequently. Orthostatic hypotension can often be managed through lifestyle changes such as staying hydrated and avoiding alcohol or caffeine, while medications may also be prescribed in severe cases. Cardiac syncope requires immediate medical attention as it can indicate a serious underlying heart condition that requires treatment.
It’s important for individuals who experience episodes of syncope to seek medical evaluation from their healthcare provider to determine the type and underlying cause of their symptoms so that appropriate treatment can be administered if necessary.
Causes
Syncope, commonly known as fainting, is a medical condition that causes a temporary loss of consciousness and muscle strength due to inadequate blood flow to the brain. There are various causes of syncope, including physical or emotional stress, dehydration, standing for prolonged periods, certain medications like diuretics and blood pressure drugs, heart conditions such as arrhythmias and valve disorders, and neurological disorders such as Parkinson’s disease and epilepsy. Additionally, low blood sugar levels can also lead to syncope in people with diabetes.
Another common cause of syncope is vasovagal syncope which occurs when there is a sudden drop in heart rate and blood pressure triggered by a specific stimulus like pain or emotional distress. This type of syncope usually does not require medical treatment unless it occurs frequently or results in injury from falls. In rare cases, syncope can be caused by more serious underlying conditions such as pulmonary embolism or heart attack.
It is important to identify the underlying cause of syncope in order to provide appropriate treatment. Patients who experience recurrent episodes of fainting should seek medical attention immediately for proper diagnosis and management.
Symptoms
Syncope, also known as fainting or passing out, is a sudden loss of consciousness caused by a temporary drop in blood flow to the brain. Symptoms of syncope include dizziness, lightheadedness, blackout headaches, and blurred vision. Some individuals may also experience feelings of nausea or sweating before losing consciousness. In some cases, individuals may experience seizures or convulsions after fainting.
It is important to note that syncope can be caused by various underlying medical conditions such as heart problems, low blood sugar levels, and dehydration. Therefore, it is crucial to seek immediate medical attention if you experience frequent episodes of fainting or if your symptoms are severe and prolonged.
In conclusion, recognizing the warning signs and symptoms of syncope can help prevent injuries and complications associated with fainting episodes. If you experience any symptoms of syncope or have concerns about your overall health and well-being, it is recommended that you reach out to your healthcare provider for further evaluation and treatment options.
Diagnosis
When it comes to diagnosing syncope, there are several steps that a healthcare provider may take. The first step is typically a thorough physical exam and medical history review. This can help the provider identify any potential underlying conditions or risk factors that could be contributing to the patient’s syncope episodes.
After this initial assessment, additional diagnostic tests may be ordered. These could include blood tests, electrocardiograms (ECGs), echocardiograms, or tilt table tests. In some cases, imaging studies like MRIs or CT scans may also be necessary in order to rule out structural issues within the brain or cardiovascular system.
Overall, an accurate diagnosis of syncope is essential in order to develop an effective treatment plan and prevent future episodes from occurring. By working closely with their healthcare team and undergoing any necessary testing, patients can feel confident that they are receiving the most comprehensive care possible for this potentially concerning condition.

Treatment
One of the most common treatments for syncope, also known as fainting, is avoidance of triggers. If a person is prone to fainting due to certain activities or situations, it is important to avoid them as much as possible. This may include standing for long periods of time, exposure to heat or dehydration, and sudden changes in position.
In some cases, medications may be prescribed to help prevent syncope episodes. These medications work by regulating blood pressure and heart rate. They are typically used in cases where avoiding triggers is not enough to prevent fainting spells.
If an individual experience frequent episodes of syncope despite these measures, more invasive treatment options may be necessary. These can include implantable devices like pacemakers or defibrillators that regulate heart rhythms and electrical impulses. In severe cases where other treatments have failed, surgery may be required to identify and correct underlying issues causing the fainting spells.
Prevention
Prevention is crucial when it comes to syncope, which is a sudden loss of consciousness caused by a lack of blood flow to the brain. The best way to prevent syncope is by identifying its underlying cause and treating it appropriately. This may involve changing medications that are causing low blood pressure, addressing dehydration or anemia, or managing heart conditions. Additionally, avoiding triggers such as hot environments, standing for long periods of time without moving around, or consuming alcohol can also help prevent syncope.
In some cases, lifestyle changes such as increasing fluid and salt intake or wearing compression stockings may be recommended to improve blood flow and prevent syncope episodes. It’s important to work closely with a healthcare provider to develop an individualized plan for preventing syncope based on the underlying cause and any coexisting medical conditions. By taking proactive measures and making necessary adjustments in daily routines and habits, individuals living with syncope can significantly reduce their risk of experiencing episodes of fainting and associated complications such as injuries from falls.
Conclusion
In conclusion, syncope is a common yet often overlooked medical condition that can have serious consequences if left untreated. While many individuals may experience fainting spells at some point in their lives, recurrent episodes of syncope should never be ignored or taken lightly. It is important to consult with a healthcare provider for proper diagnosis and management of this condition.
Treatment options for syncope vary depending on the underlying cause and can range from lifestyle modifications to medication or even surgery in severe cases. It is essential for patients with syncope to work closely with their healthcare team to identify triggers, implement preventive measures, and monitor symptoms over time.
Overall, recognizing the signs and symptoms of syncope early on can greatly improve outcomes and quality of life. By taking an active role in managing this condition through regular check-ups and open communication with healthcare providers, patients can achieve better control over their health and reduce the risk of long-term complications.
Published on May 16, 2023 and Last Updated on October 22, 2025 by: Mayank Pandey