If you’ve recently had surgery or been ill, you may have been warned about developing a condition called Atelectasis. You might be feeling short of breath, a little feverish, or have a persistent cough. While the name sounds intimidating, atelectasis is a very common and usually reversible lung condition.
It’s a frequent complication after surgery, but it’s important to understand what it is, why it happens, and how to treat it. This guide will cover the causes, symptoms, and the simple, effective treatments to help you recover.
Table of Contents
What Is Atelectasis?
Atelectasis is the medical term for a partial lung collapse. It does not mean your entire lung has collapsed (which is typically a pneumothorax). Instead, atelectasis happens when the tiny, elastic air sacs in your lungs, called alveoli, deflate and fail to inflate properly.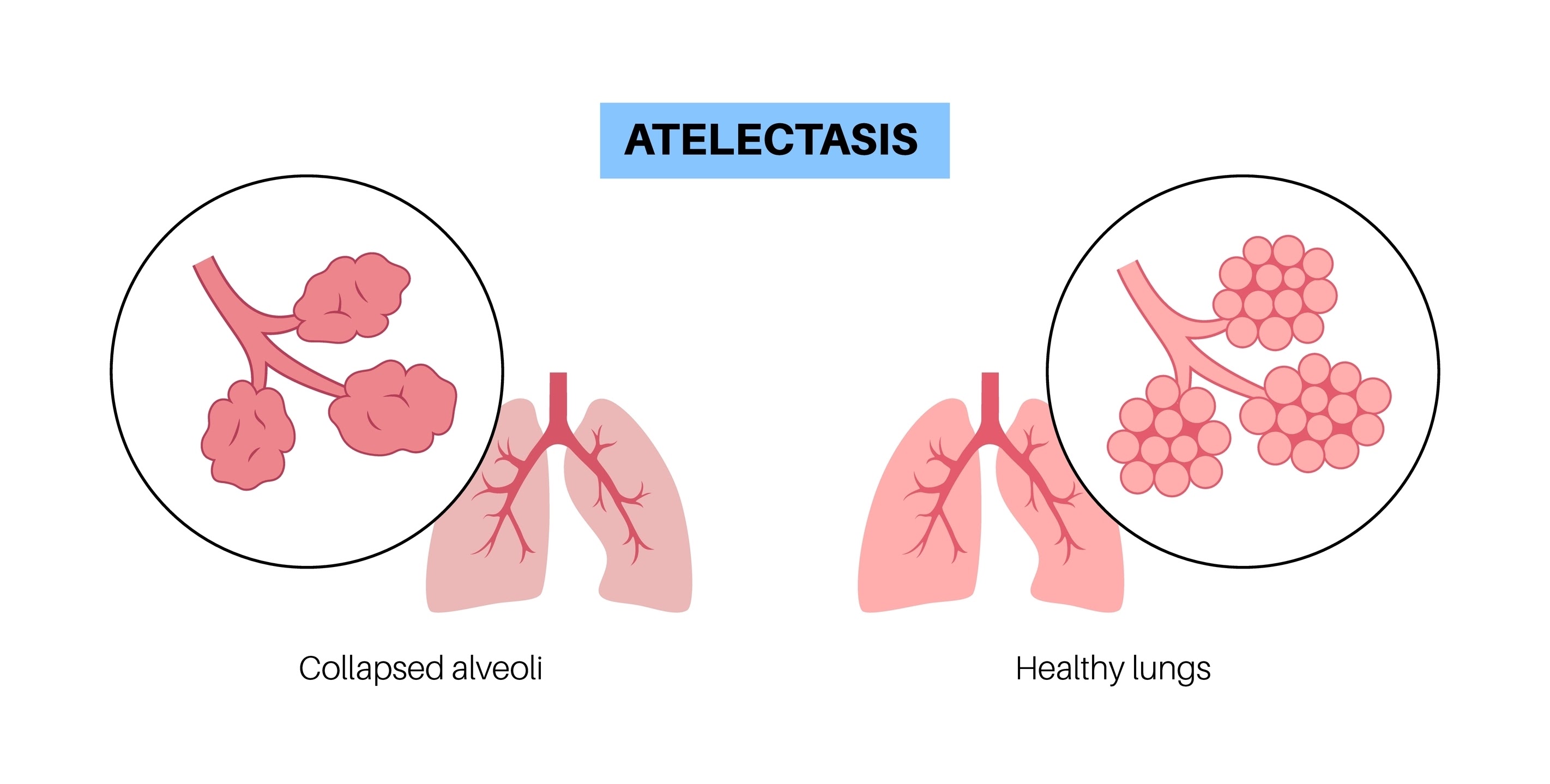
When your alveoli can’t fill with air, they can’t deliver enough oxygen to your blood. This can cause a dip in your oxygen levels and lead to symptoms like shortness of breath. While a small area of atelectasis may cause no symptoms, a larger area can be serious, potentially leading to complications like pneumonia.
Common Causes of Atelectasis
Atelectasis is caused by two main issues: a blockage in your airway (obstructive) or pressure from outside the lung (non-obstructive).
Obstructive Atelectasis
This happens when something physically blocks the air from reaching your alveoli. Common blockages include:
- Mucus Plug: This is the most common cause. After surgery or during a severe respiratory illness, mucus can build up and form a “plug” in an airway.
- Foreign Object: Accidentally inhaling an object (like a small piece of food) can block an airway.
- Tumor: A growth inside the airway can block airflow.
Non-Obstructive Atelectasis
This type is caused by pressure or other factors that make it difficult for the lung to expand.
- Post-operative Atelectasis: This is the most frequent type. It’s a combination of factors:
- Anesthesia: General anesthesia affects your normal breathing patterns and urge to cough.
- Shallow Breathing: Pain after surgery (especially in the chest or abdomen) makes you take short, shallow breaths.
- Being Bedridden: Lying in one position for a long time makes it harder for your lungs to expand fully.
- Pleural Effusion: A buildup of fluid in the space between your lungs and your chest wall can press on the lung, causing it to collapse.
- Tumor: A tumor outside the lung can push on it.
- Pneumothorax: This is when air leaks into the space between your lung and chest wall, which can cause the lung to collapse. While a different condition, it can lead to atelectasis.
- Lung Scarring: Damage from previous infections or lung diseases.
Key Symptoms of Atelectasis
If only a small area of your lung is affected, you may have no symptoms at all. However, if a larger area is involved, the atelectasis symptoms are a direct result of your body not getting enough oxygen.
Symptoms can include:
- Shortness of breath (dyspnea)
- Rapid, shallow breathing
- A persistent cough
- Low-grade fever (very common after surgery)
- Chest pain (less common)
Risk Factors
Your risk of developing atelectasis is higher if you:
- Have recently had surgery with general anesthesia, especially chest or abdominal surgery.
- Are a smoker (smoking damages your lungs and increases mucus production).
- Have lung diseases like asthma, COPD, or cystic fibrosis.
- Are obese, as excess weight can press on the lungs.
- Have a condition that causes prolonged bed rest or difficulty breathing deeply.
- Have a neuromuscular condition (like muscular dystrophy) that weakens breathing muscles.
Diagnosis
If your doctor suspects atelectasis based on your symptoms and recent medical history (like a surgery), they will start with a physical exam.
- Physical Exam: Your doctor will listen to your chest with a stethoscope. Areas of atelectasis will have decreased or absent breath sounds.
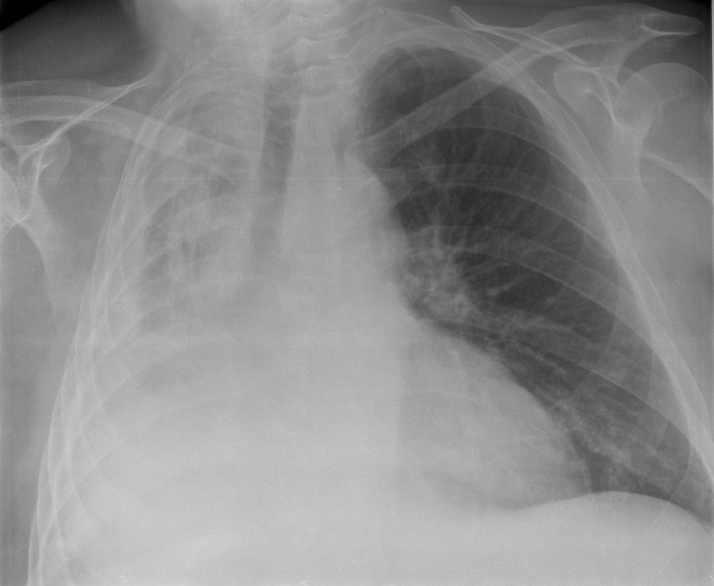
- Chest X-ray: This is the most common and effective way to confirm the diagnosis. The collapsed area will appear as a white, dense (opaque) patch.
- Pulse Oximetry: A small device clipped to your finger will measure your blood oxygen level, which may be low.
- CT Scan: A CT scan provides a more detailed image and can help your doctor see the blockage or pressure point that is causing the collapse.
- Bronchoscopy: If a blockage is suspected, your doctor may use a bronchoscope (a thin, flexible tube with a camera) to look inside your airways and potentially remove a mucus plug.
Treatment Options for Atelectasis
The main goal of treatment for atelectasis is to re-expand the collapsed alveoli. The good news is that this is often achieved with simple, non-invasive techniques.
Breathing and Physical Therapies
These are the cornerstones of treatment, especially for post-operative atelectasis.
- Deep Breathing Exercises: You will be taught to take slow, deep breaths and hold them for a few seconds to help “pop” open the alveoli.
- Incentive Spirometer: This is a plastic device you breathe into. According to the American Lung Association, using it 10 times every hour you’re awake is a highly effective way to re-expand your lungs.
- Chest Physiotherapy: This involves techniques like percussion (clapping) on your back over the collapsed area to loosen mucus.
- Postural Drainage: Your therapist may position you so that gravity helps drain mucus from your lungs.
Medications
- Bronchodilators: If you have asthma or COPD, an inhaler may be used to open your airways.
- Mucolytics: Medications to thin your mucus (like Mucomyst) may be given via a nebulizer.
Surgical or Procedural Treatments
If the above methods don’t work, or if there is a clear blockage:
- Bronchoscopy: As mentioned in diagnosis, a doctor can use the bronchoscope to suck out a mucus plug or remove a foreign object.
- Treating the Cause: If the atelectasis is from a pleural effusion or tumor, the underlying condition must be treated (e.g., draining the fluid).
Prevention Tips
The best way to deal with atelectasis is to prevent it, especially if you are having surgery.
- Before Surgery: If you smoke, quit at least 6-8 weeks before your operation.
- After Surgery:
- Use your incentive spirometer as directed.
- Cough and breathe deeply. Hold a pillow over your incision for support.
- Get up and walk (ambulate) as soon as your medical team says it’s safe.
- Manage your pain. If it hurts too much to breathe, you won’t. Talk to your nurse about pain medication.
When to See a Doctor
Seek emergency medical care (call 911) if you experience:
- Sudden, severe shortness of breath
- Severe chest pain
- Bluish discoloration of your lips or fingernails (cyanosis)
Call your doctor if you are recovering from surgery or illness and develop:
- Worsening shortness of breath
- A new fever
- A cough that won’t go away
Atelectasis is common, but it’s important to treat it seriously to prevent complications and get you back to breathing easy.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified healthcare professional for any health concerns or before making any decisions related to your health or treatment.
Published on August 7, 2023 and Last Updated on October 30, 2025 by: Priyank Pandey