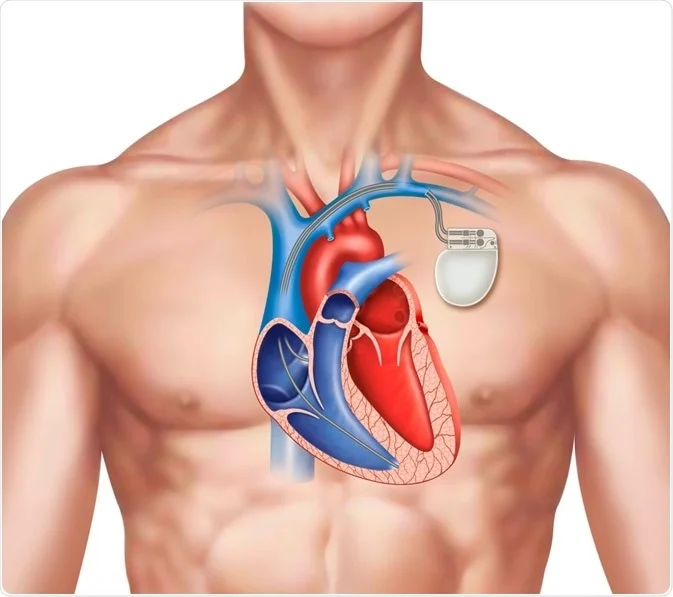
A pacemaker is a small device that helps regulate an individual’s heart rate by sending electrical impulses to the heart. It is typically implanted just beneath the skin, usually near the collarbone, and connected to the heart through thin wires called leads. While often associated with elderly individuals, pacemakers can be necessary for people of all ages who have irregular or slow heart rhythms.
One interesting aspect of pacemakers is their ability to adapt to the needs of each patient. Modern pacemakers are designed with advanced technology that allows them to adjust the pacing rate based on a person’s activity level. This means that if someone with a pacemaker engages in physical exercise or experiences stress, it will automatically detect these changes and increase the pacing rate accordingly.
In addition to providing assistance for irregular heart rhythms, some pacemakers also come equipped with other useful features. For instance, some devices have sensors that monitor respiratory patterns and adjust heart rates accordingly, helping individuals breathe more efficiently during sleep. Imagine how intriguing it would be for such a tiny device not only to keep your heartbeat steady but also to listen closely enough to sense when you’re breathing and how fast! Pacemakers are not just life-saving devices; they are incredibly intelligent gadgets that constantly work behind the scenes to optimize cardiac health.
Table of Contents
History
The development of pacemakers is a fascinating journey through the history of medical advancements. The first pacemaker, introduced in the 1950s, was a large and bulky device that required external power and wires to be inserted into the heart. However, over time, with technological innovations and miniaturization efforts, pacemakers have evolved into small implantable devices that can be easily placed under the skin.
One major breakthrough came in the 1960s when battery-operated pacemakers were developed. This allowed patients more mobility and eliminated the need for external power sources. Another significant advancement occurred in the early 1990s with the introduction of rate-responsive pacemakers. These devices are able to adjust heart rates according to physical activity levels, providing patients with a more natural cardiac rhythm and improved quality of life.
The future of pacemakers looks promising as researchers continue to explore new ways to enhance their capabilities. One current area of focus is on wireless communication technology which will eliminate the need for electrode leads altogether, making it even easier for patients to receive life-saving treatment without invasive procedures. With each leap forward in technology, pacemakers continue to evolve and improve, offering hope for millions around the world suffering from cardiac arrhythmias.
How does it work?
One of the most vital aspects of a pacemaker’s functionality lies in its ability to send electrical signals to the heart and regulate its rhythm. This process is often referred to as pacing. When the natural electrical signals produced by the heart fail to maintain a steady heartbeat, a pacemaker steps in by generating small amounts of electricity in strategic timings. These electric impulses are delivered through one or more wires, also known as leads, which are attached directly to the heart muscle.
To better understand how this works, it is crucial to delve into the intricate mechanisms behind electrical signaling within our bodies. The natural rhythm of the heart is controlled by tiny clusters of specialized cells called sinoatrial (SA) nodes and atrioventricular (AV) nodes. The SA node serves as your heart’s primary natural pacemaker, while the AV node acts as a gatekeeper between your atria and ventricles—allowing them to contract with proper synchronization. A malfunctioning SA or AV node can disrupt this delicate coordination and lead to an irregular heartbeat or arrhythmia. In such cases, a pacemaker can take over by continuously sending electrical signals in order to maintain regular contractions and keep your blood pumping efficiently throughout your body.
Overall, understanding how electrical signaling works within our hearts provides us with profound insights into how lifesaving devices like pacemakers function.
Types of pacemakers
There are several types of pacemakers available to treat various heart conditions. One commonly used type is the single-chamber pacemaker. As the name suggests, this pacemaker has only one lead, which is placed either in the right atrium or the right ventricle of the heart. The single-chamber pacemaker sends electrical signals to regulate heart rate and rhythm.
Another type of pacemaker is the dual-chamber pacemaker. This device has two leads that are implanted in both the right atrium and right ventricle of the heart. By monitoring and stimulating both chambers, a dual-chamber pacemaker can more effectively coordinate contractions and optimize blood flow through each phase of the cardiac cycle.
In addition to single and dual chamber pacemakers, there are also biventricular (or CRT) devices that have three leads – one in each atrium and another in the left ventricle. These specialized devices are used specifically for individuals with heart failure or certain cardiac arrhythmias that require synchronization between all three chambers for optimal functioning.
Each type of pacemaker offers its own advantages based on an individual’s specific needs and condition. It is important for patients to work closely with their healthcare provider to determine which type of pacemaker would best address their unique circumstances and help them maintain a healthy heart rhythm.
Indications for pacemaker implantation
Pacemakers are small, battery-operated devices that help regulate the heartbeat by using electrical pulses to stimulate the heart muscle. They are typically implanted in individuals who have heart conditions that affect the normal functioning of the heart’s electrical system. One common indication for pacemaker implantation is bradycardia, which is defined as an abnormally slow heart rate. This can occur due to aging, damage to the heart’s electrical pathways, or as a side effect of certain medications.
Another condition that may require a pacemaker is sick sinus syndrome (SSS), which refers to dysfunction in the sinoatrial node – the natural pacemaker of the heart. SSS often leads to alternating episodes of rapid and slow heart rates, causing symptoms such as dizziness, fatigue, and shortness of breath. A pacemaker can help maintain a stable and regular heartbeat for individuals with this condition.
Thirdly, individuals who have experienced certain types of cardiac arrhythmias may also require a pacemaker. Arrhythmias such as complete heart block or atrioventricular (AV) block can disrupt the flow of electrical impulses between the upper chambers (atria) and lower chambers (ventricles) of the heart. By implanting a pacemaker, these abnormal conduction patterns can be corrected, ensuring proper coordination between atria and ventricles and maintaining an adequate heartbeat.
Ultimately, indications for pacemaker implantation are based on individual patient characteristics and specific abnormalities in their cardiac rhythms.
Procedure
Implanting a pacemaker is a critical procedure that involves positioning a tiny device under the skin to help regulate an individual’s heartbeat. Throughout the process, patient safety remains paramount as medical professionals undertake careful planning and meticulous execution. Firstly, an incision is made just below the collarbone after administering local anesthesia to numb the area. Through this opening, leads are guided into specific chambers of the heart while monitoring optimal placement with advanced imaging technology. Once secured, these leads connect to the pacemaker device itself.
The advancements in technology have led to smaller and more sophisticated pacemakers being developed over time. Modern pacemakers offer various programmable features like rate-responsive pacing and dual-chamber functions, resulting in more tailored treatments for patients with distinct requirements. Additionally, many new models come equipped with wireless technology that allows remote monitoring of heart activity by healthcare providers. This seamless interaction enables doctors to provide proactive healthcare and make any necessary adjustments without patients having to visit a clinic.
Pacemaker implantation offers hope for individuals suffering from cardiac conditions by providing them with reliable support that can significantly enhance their quality of life. As medical knowledge continues to advance alongside technological developments, it is certain that future generations will benefit from even more refined devices and procedures. The implantation process exemplifies both the commitment of medical professionals to their patient’s well-being and the continuous efforts made towards improving cardiac care for all individuals in need.
Risk and side effects
One of the factors that many patients consider when deciding whether to get a pacemaker is the potential risks and side effects associated with the procedure. While pacemakers are generally considered safe and well-tolerated, like any medical intervention, there are risks involved. These can include infection at the implantation site, bleeding or bruising in the area surrounding the device, damage to blood vessels or nerves during insertion, or an allergic reaction to the materials used in the pacemaker.
It’s important for patients to have an open and honest discussion with their doctor about these potential risks before undergoing pacemaker implantation. Understanding these possibilities allows individuals to make informed decisions about their own health care. By weighing these risks against the benefits of a pacemaker, such as improved heart function and quality of life, patients can gain greater confidence in their decision-making process and feel more empowered throughout their treatment journey. Ultimately, it’s crucial to remember that while there may be risks involved with any medical procedure, advancements in technology and expertise in cardiology have significantly reduced many of these concerns related to pacemakers.
Conclusion
In conclusion, advancements in pacemakers have revolutionized the treatment of heart conditions and have significantly improved the quality of life for patients worldwide. The introduction of wireless technology and miniaturization has made it possible for pacemakers to be smaller, more efficient, and less invasive than ever before. Additionally, the incorporation of advanced sensors and algorithms has allowed for more personalized and precise control over heart rhythms.
Looking toward the future, there are several exciting prospects on the horizon for pacemaker technology. Researchers are exploring the use of renewable energy sources to power these devices, potentially eliminating the need for battery replacements altogether. Furthermore, advancements in artificial intelligence may enable pacemakers to not only monitor heart rhythms but also detect early signs of potential complications or changes in overall health. This could lead to proactive interventions that can prevent serious cardiac events before they even occur.
As we continue to innovate and improve upon existing technologies, one thing remains certain: pacemakers will play a vital role in managing heart conditions and prolonging lives well into the future. With ongoing research and development efforts focused on enhancing performance, increasing longevity, and reducing risks associated with these devices, we can look forward to a future where individuals living with heart conditions can lead healthy, active lives without skipping a beat.
Published on August 17, 2023 and Last Updated on August 17, 2023 by: Mayank Pandey