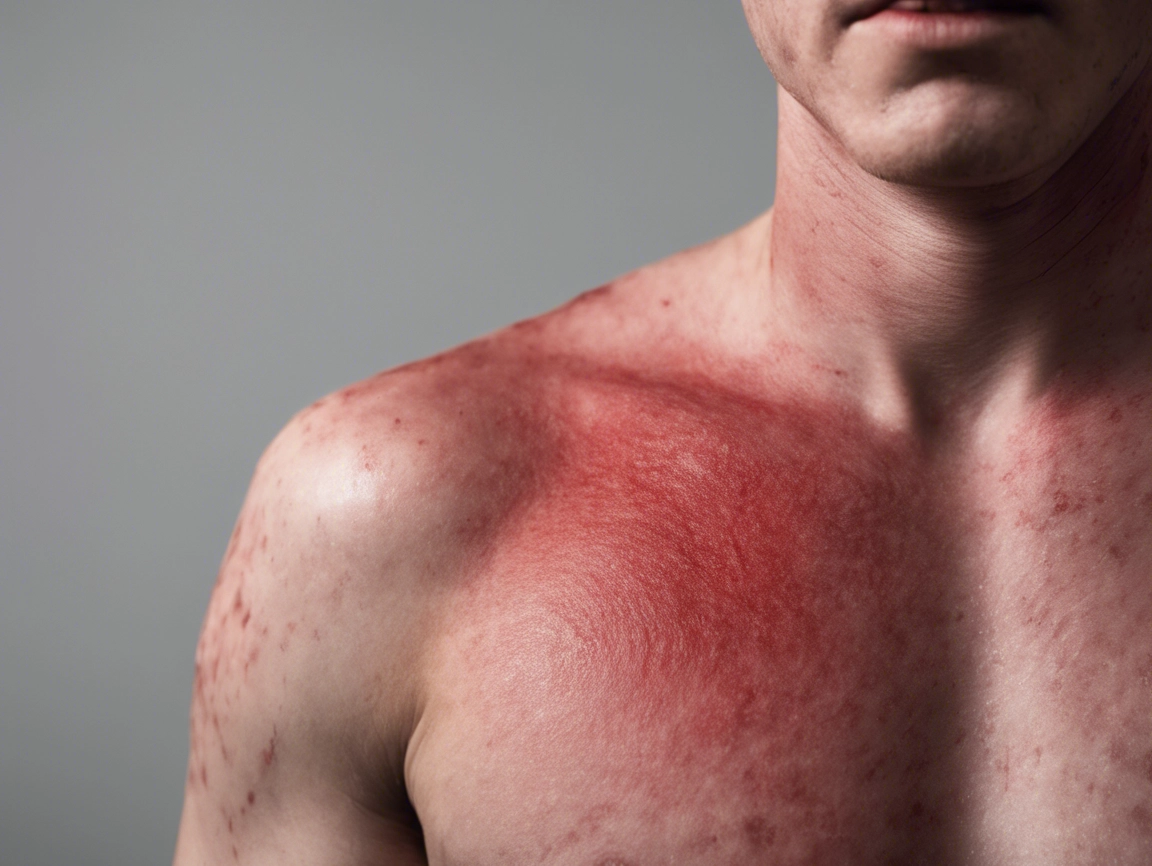
Finding a new, itchy, circular rash on your skin can be alarming, especially when you hear it might be Ringworm. The name is a major source of confusion, so let’s clear this up first: Ringworm is not caused by a worm of any kind.
It is a very common, highly contagious fungal infection of the skin. Because the rash often appears in a ring-like or circular pattern, it was once mistakenly thought to be caused by a worm, and the misleading name stuck. This guide will walk you through what’s really happening, the symptoms, and the simple, effective treatments.
Table of Contents
What Is Ringworm?
Ringworm is a skin infection caused by a common type of fungus called a dermatophyte. These tiny organisms live on the dead tissues of your skin, hair, and nails.
The medical term for ringworm on the body is tinea corporis. The “tinea” name changes depending on where the infection is:
- Tinea pedis: Athlete’s foot (on the feet)
- Tinea cruris: Jock itch (in the groin)
- Tinea capitis: Scalp ringworm (on the head)
This article will focus on tinea corporis (ringworm on the body), but the causes and treatments are very similar.
Common Causes of Ringworm (How Is It Spread?)
What causes ringworm? As a fungal infection, it spreads through contact. According to the Centers for Disease Control and Prevention (CDC), you can get ringworm in a few key ways:
- Human-to-Human: This is a very common way it spreads. Direct, skin-to-skin contact with an infected person can pass the fungus to you.
- Animal-to-Human: You can get ringworm from infected pets. Cats (especially kittens) and dogs are common carriers. You can also get it from farm animals like cattle.
- Object-to-Human: The fungus can live on surfaces and objects for a long time. You can get infected by touching:
- Contaminated towels, bedding, or clothes
- Combs or brushes
- Surfaces in locker rooms or public showers
- Gym equipment
Key Symptoms of Ringworm
The classic sign of ringworm is the rash, which typically appears 4 to 14 days after your skin comes in contact with the fungus.
Symptoms include:
- An itchy, circular rash
- The rash often has a raised, scaly border that is redder than the center
- The center of the ring may be clear, scaly, or have a few bumps
- The rash can grow, and you may develop one or more overlapping rings
- It can be mildly to intensely itchy
On the scalp (tinea capitis), it may look like a scaly, bald patch. On the feet (athlete’s foot), it often appears as peeling, cracked, and itchy skin between the toes.
Diagnosis
A doctor can often diagnose ringworm just by looking at it. To confirm the diagnosis and rule out other conditions like eczema or psoriasis, they may perform a simple, painless test:
- Skin Scraping (KOH Test): Your doctor will scrape a small amount of the scaly rash onto a slide, add a drop of potassium hydroxide (KOH), and look at it under a microscope. The KOH solution dissolves the skin cells, making the fungal cells easy to see.
Treatment Options for Ringworm
The good news is that ringworm is highly treatable. For most cases on the skin, over-the-counter (OTC) treatments are very effective.
Over-the-Counter (OTC) Antifungals
Look for a ringworm treatment cream, lotion, or powder. These products don’t “kill” the fungus instantly but stop it from growing, allowing your skin to heal. Common ingredients include:
- Clotrimazole (e.g., Lotrimin)
- Miconazole (e.g., Micatin)
- Terbinafine (e.g., Lamisil AT)
Crucial Tip: You must follow the directions exactly. The American Academy of Dermatology (AAD) emphasizes that you should continue to apply the cream for 1 to 2 weeks after the rash disappears. This is to kill any remaining fungus and prevent it from coming back.
Prescription Treatments
You will need to see a doctor for prescription-strength treatment if:
- The OTC creams are not working after 2 weeks.
- The infection is widespread or severe.
- The infection is on your scalp (tinea capitis). Ringworm on the scalp almost always requires oral, prescription antifungal pills (like terbinafine or fluconazole) to get deep into the hair follicle.
Risk Factors
Is ringworm contagious? Yes, it is very contagious. You are at a higher risk of getting it if you:
- Are an athlete, especially in contact sports (wrestling, football)
- Use public locker rooms or showers
- Live in a warm, humid climate
- Sweat heavily
- Have close contact with an infected person or animal
- Have a weakened immune system
Prevention Tips
You can prevent ringworm by practicing good hygiene.
- Keep your skin clean and dry. Dry off completely after showering.
- Don’t share. Avoid sharing towels, combs, brushes, clothes, or other personal items.
- Wear shower shoes. Use flip-flops in public showers, locker rooms, and pool areas.
- Wash your hands. Always wash your hands after playing with pets.
- Check your pets. If your pet has a patch of missing fur, take them to the vet to be checked.
- Wash contaminated items. Wash bedding and any clothes that may have touched the infection in hot, soapy water.
When to See a Doctor
While many cases of ringworm can be handled at home, you should make an appointment with your doctor if:
- The rash does not start to improve after 1-2 weeks of using an OTC antifungal cream.
- The rash is spreading, getting redder, or getting more painful.
- You see signs of a secondary bacterial infection (like pus, significant swelling, or fever).
- You have ringworm on your scalp. This requires a doctor’s diagnosis and prescription oral medication.
- You have a weakened immune system (due to a condition like diabetes, HIV, or cancer treatment).
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified healthcare professional for any health concerns or before making any decisions related to your health or treatment.
Published on July 25, 2023 and Last Updated on October 30, 2025 by: Priyank Pandey